Arthritis of the Hand, Thumb & Wrist
Arthritis at the base of thumb is a very common disorder encountered by the primary care physician and the hand specialist. It is referred to by many different names: basal joint arthritis, first CMC (carpometacarpal) arthritis, and trapezio-metacarpal arthritis.
Did You Know?
It is the second most common arthritic problem encountered in the hand, behind distal interphalangeal joint arthritis. However, it is the most common site for which surgery is sought because of its profound impact on hand function. The joint is particularly susceptible to wear because of the tremendous physical stresses placed on it throughout life. Pinch pressures at the thumb tip are magnified approximately tenfold at the CMC joint. Women are affected more commonly than men, related to postmenopausal ligamentous laxity. The problem presents sometime in the fourth through sixth decades. It may be seen earlier in life, usually associated with prior trauma to the joint.
Diagnosis
The differential diagnosis of CMC arthritis includes other common disorders at the radial aspect of the hand and wrist. DeQuervain’s tenosynovitis may mimic symptoms of CMC arthritis. Also, arthritis involving the radial styloid or the STT (scaphotrapezialtrapezoidal) joint may also cause pain similar to CMC arthritis. The diagnosis is made by history, physical exam, and radiographic findings. Patients typically complain of aching and pain involving the thenar aspect of the hand and base of the thumb. Pinching, removing jar lids, turning doorknobs or even the keys to the car may be problematic. Patients who are involved in jobs that require significant pinching and grasping activities may have exacerbation of the condition. During the physical exam, there is often some swelling or prominence noted at the dorsal base of the thumb. This is a sign of subluxation of the first metacarpal at the CMC joint. One of the definitive physical findings is that of a positive “grind test.” The first metacarpal is held firmly and pushed proximally to load the joint while manipulating the base of the metacarpal in different directions. This will reproduce the patient’s symptoms and also usually elicit some palpable crepitus in the joint. DeQuervain’s tenosynovitis on the other hand, results in specific tenderness more proximal, over first dorsal compartment tendons near the radial styloid. If after the history and physical exam, there still is some question regarding the diagnosis, radiographs should help confirm the problem. Three standard views of the thumb are usually sufficient to evaluate the joint.
The Findings
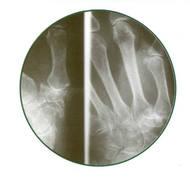
Figure 1
Typical findings are loss of joint space, spurring and osteophyte formation from the trapezium and metacarpal base. (Figure 1) There may be more extensive involvement around the trapezium, including the scaphotrapezial joint (pan trapezial arthritis). One thing to keep in mind is that radiographic findings do not always correlate well with physical findings or symptoms. We frequently see patients with incidental findings of end stage disease on x-rays that have no symptoms. Likewise very minimal or subtle findings on x-ray can be associated with significant pain and disability.
Treatment Options
Treatment begins with conservative measures. Anti-inflammatories may alleviate symptoms adequately. Splints that immobilize or support the CMC joint may be purchased or custom-made by a therapist to help patients during certain exacerbating activities. A corticosteroid injection can often relieve pain significantly but is often only a temporizing procedure. When conservative methods are no longer effective and the pain is disabling, surgical arthroplasty remains a time-honored successful procedure for this problem.
There are numerous procedures described including:
- Wrist Tenotomy
- Replacement of the trapezium with titanium or silicone and an array of arthroplasties utilizing tendon with or without use of an implant called a tightrope
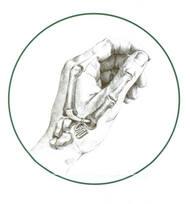
Figure 2
Most surgeons today prefer some type of tendon interposition arthroplasty, using either the Flexor Carpi Radialis (FCR) or the Abductor Pollicis Longus tendon (APL). The idea behind the procedure is to remove the opposing arthritic surfaces (the trapezium excision) and then provide some type of suspension of the remaining metacarpal base. (Figure 2) The procedure is usually performed under a general anesthetic in an outpatient setting and takes about one hour. Post-operatively, a thumb spica splint is worn for 6 weeks continuously followed by range of motion exercises and therapy under the guidance of an experienced hand therapist. Typically, patients return to unrestricted activity at 10-12 weeks.
Results
Of all the procedures performed by hand surgeons, this one ranks very high in terms of patient satisfaction. All of the various procedures described above have shown good results overall. Satisfaction in terms of pain relief and return to activity range from 80-98% depending on the studies cited. Most patients can resume their normal activities without restriction. In some cases, where demand is heavy in terms of gripping and pinching (heavy laborers), a fusion of the CMC joint may be preferred over the arthroplasty. This is thought to hold up better in the high demand hand. For most of the population, however, the arthroplasty is the procedure of choice. At Orthopaedic Associates of Michigan, we have extensive experience in treatment of CMC arthritis of the thumb. We continue to evaluate and integrate some of the newer methods of the arthroplasty procedure. Our therapy department is instrumental in the treatment plan, beginning with conservative treatment, splint application, and following through with post-operative therapy and rehabilitation.


