Hand Infections
Primary care physicians and emergency room physicians are frequently confronted with hand infections. Gout, pseudogout, and acute synovitis can mimic infection. A reasonable knowledge of the spectrum of hand infections is necessary for recognition and proper initial treatment. Delayed or inadequate treatment can result in the progression of a simple process to a limb threatening or even life threatening situation.
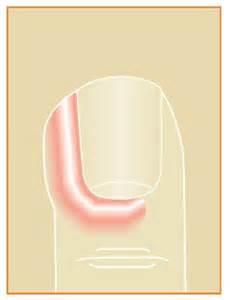
Paronychia (Nailfold Infection)
Paronychial infections are common and account for 10 to 20 percent of hand infections.
What Causes Hand Infections?
- Hangnail, nail biting and frequent exposure to moisture are common contributing factors.
- Dry cracked skin due to cold dry weather or detergents also play a part.
Treatment Options
- Gently probing the involved nailfold usually provides adequate drainage.
- Daily soaks and oral antibiotics are recommended for several days.
Staphylococcus aureus is the usual organism. Pus under the nail plate requires removal of all or part of the nail plate.
Herpetic Whitlow
Herpes simplex infection of the fingertip tissues can mimic paronychia.
Symptoms
Pain is usually severe and clear fluid filled vesicles follow the initial phase of swelling and redness. Viral cultures of the vesicle fluid confirm the diagnosis.
Treatment Options
Treatment is non-operative unless there is a secondary infection. Antiviral drugs may shorten the several-day course of infection. Latent infection may result in several recurrences over a period of weeks to months.
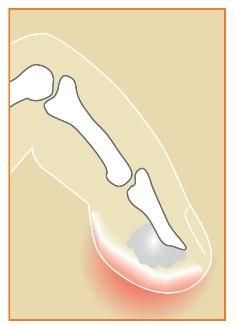
Felon
A felon is an abscess of the fingertip pad.
Symptoms
Minimal trauma can provide an entry point for bacteria, usually staphylococcus aureus. Swelling, redness, and intense pain develop.
Treatment Options
Drainage through a longitudinal incision over the point of maximal tenderness provides relief. The infection resolves promptly with drainage and appropriate antibiotics. Residual fingertip tenderness can be a problem.
Pyogenic Flexor Tenosynovitis
The flexor tendon sheath is a closed space containing synovial fluid. Bacteria introduced by direct trauma, or rarely as blood born pathogens, flourish in this space. Kanavel’s four classic signs below.
- fusiform digital swelling
- semiflexed digital posture
- pain with passive extension
- tenderness over the flexor tendon sheath
Treatment Options
Surgical drainage and hospitalization are required. Treatment delays can result in loss of the flexor tendons or even the digit.
Bite Wound Infections
Animal and human bite wounds commonly occur on the hand. Deep penetration of a tooth covered with a mixed flora of organisms results in cellulitis and abscess formation.
Treatment Options
Initial treatment should include irrigation and usually debridement of the puncture site. Even the tiny puncture wound from a cat’s tooth should be opened with a small stab wound. Antibiotics should be selected to cover both aerobic and anaerobic organisms. Amoxicillin/Clavulanate is recommended by many. Penicillin G and Cephalexinare are less costly. Daily wound checks are necessary and hospitalization of unreliable patients should be considered. Most clenched fist tooth puncture wounds should be explored in the operating room because the risk of infection in the metacarpophalangeal joint is very high.
Deep Space Infections of the Hand
There are five potential deep spaces within the hand:
- the inter-digital webspace between the metacarpal heads
- the thenar space
- the hypothenar space, the mid palmar space deep to the flexor tendons
- the dorsal subaponeurotic space, deep to the extensor tendons
- Parona’s space in the distal forearms deep to the digital flexor tendons
Direct penetrating trauma is the usual source of infection, although an adjacent pyogenic flexor tenosynovitis can extend into these spaces.
Symptoms
Intense pain, swelling, and limited motion in the involved digits heralds the diagnosis.
Treatment Options
Prompt drainage is critical.
Cellulitis & Fasciitis
Soft tissue infections range from non-supportive cellulitis to aggressive necrotizing fasciitis, which the general public has come to know as “flesh-eating bacteria.”
Treatment Options
Treatment of these infections range from oral antibiotics to aggressive life saving surgical debridement and hyperbaric oxygen. Treatment of these hand infections does not differ from treatment of infection in other areas of the body. Recognition leading to early treatment of hand infections can be a challenge because of the anatomy peculiar to the hand. Clinicians must maintain a high index of suspicion when evaluating patients with potential hand infections.


